Brexit risks putting social care on the critical list
Today NIESR publishes new research for the Cavendish Coalition on the implications of Brexit for the health and social care sector. Our conclusions are stark: Brexit is likely to lead to a substantial shortfall in nurses and doctors which needs to be urgently addressed by new immigration policy.
Today NIESR publishes new research for the Cavendish Coalition on the implications of Brexit for the health and social care sector. Our conclusions are stark: Brexit is likely to lead to a substantial shortfall in nurses and doctors which needs to be urgently addressed by new immigration policy. However, while the implications of any future immigration restrictions are very serious for the NHS, the much-neglected social care sector is likely to be an even greater casualty if workable immigration policies are not put in place. Here’s why.
EU migrants’ role in the social care sector
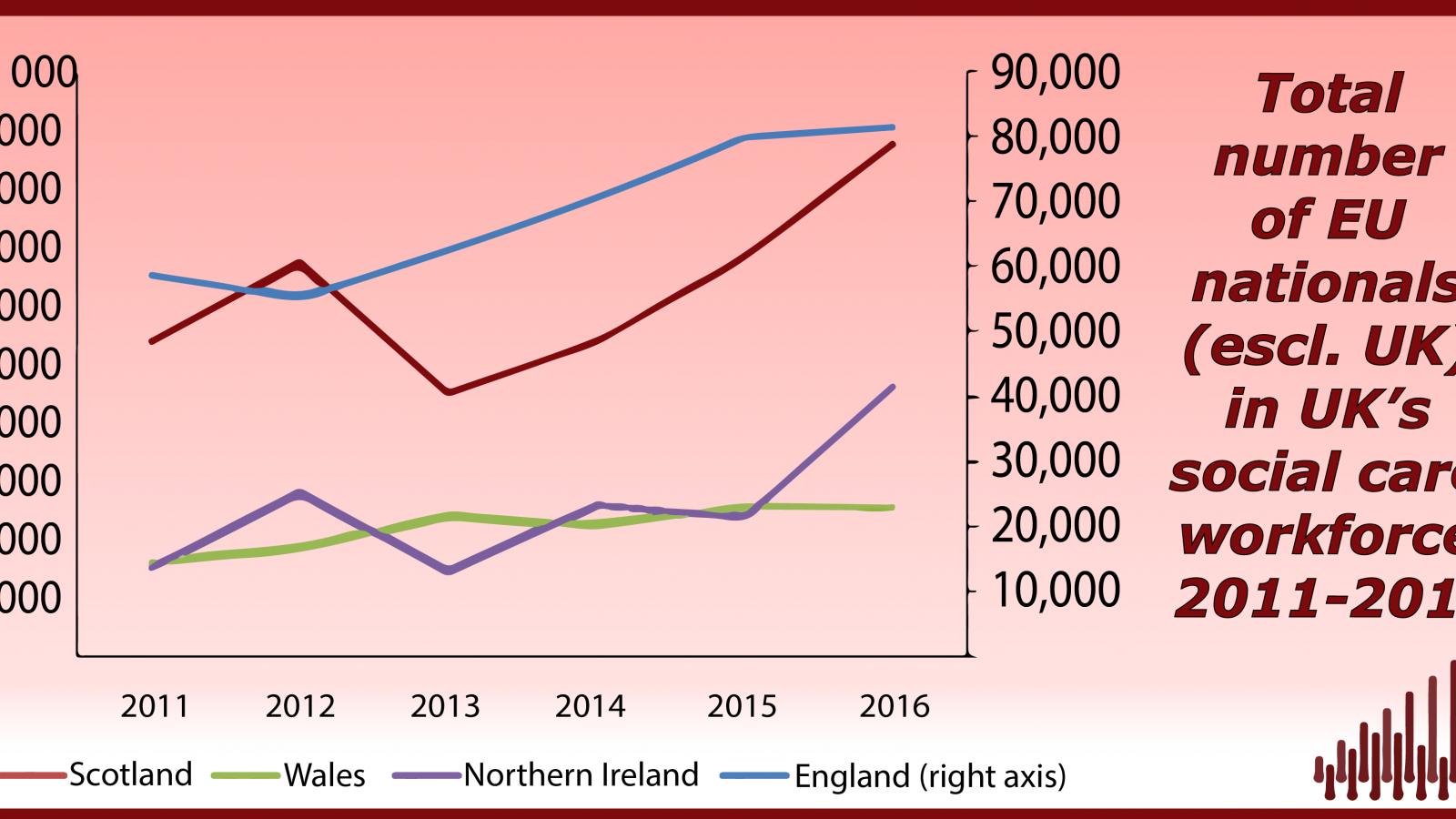
Not so long ago the social care workforce was made up largely of British women working part-time but with the rapid expansion of the sector, and competition from retail and hospitality, recruitment became more difficult. Recognising the sector’s difficulties, the points-based system (Tier 2) introduced in 2008 allowed employers to recruit some types of social care workers, for example senior staff, nurses and others categorised as skilled workers from abroad. Other visa holders such as students and domestic workers could also work in care homes. In practice, Tier 2 proved to be of limited help because numbers were capped. But fortuitously, EU migration, particularly from the EU8 countries, really took off from around 2011 and helped to fill the sector’s widening skills gap.
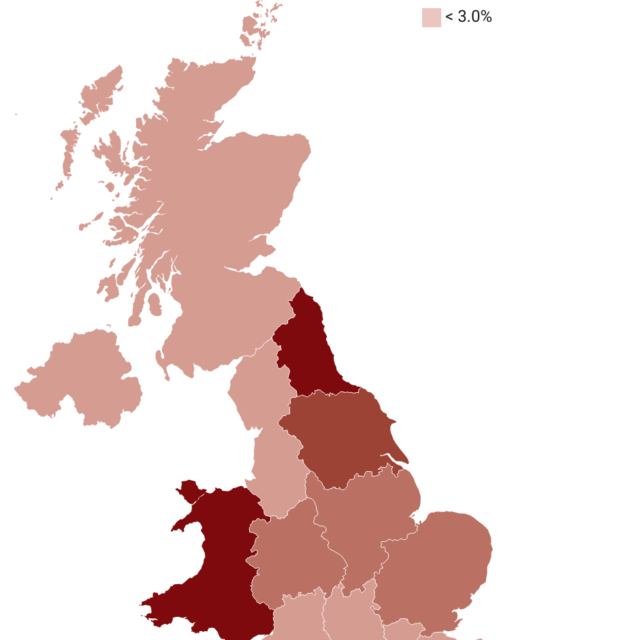
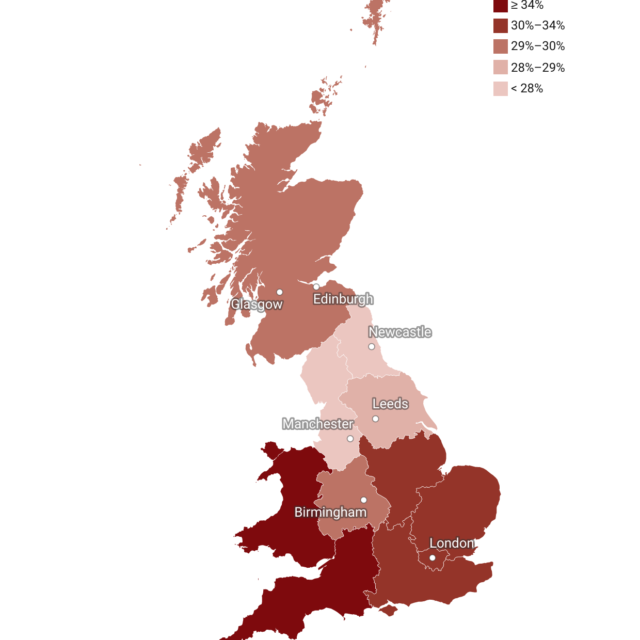
Consequently, in 2016 EU nationals made up 5.4% of the workforce (international staff from outside the EU are a further 5%). This represents an increase of 68% since 2011, during which time the proportion from outside the EU has declined in areas of the UK other than England. But despite the increase in EU migrants, the sector has continued to experience high job vacancy rates and recruitment difficulties. These have increased further since the referendum vote, and fall in net migration, with London and the South East experiencing the most serious shortages.
It’s not all about the money
Reporting in September, the Migration Advisory Committee (MAC) declined to recommend visas for social care on the grounds that its recruitment problems could be solved if wages were increased through a change in the funding model. Yet if we look at the issues faced by the sector it’s clear that there are deeper and long-standing issues which have led to dependence on migrant workers.
The sector is unattractive to British workers, especially to younger people who employers find particularly hard to recruit. The work is demanding, both mentally and physically, involving close engagement in people’s personal lives. It requires flexibility and the willingness to work at all times of the day, night, weekends and public holidays. Employers see on the job training as more important than structured training courses and the sector lacks clearly defined career routes.
Migrants seem to be less deterred by these drawbacks and probably not because money matters less to them as is often argued. Motivations of migrants often differ to other workers and they also have different characteristics which may give them an advantage in social care. They are more prepared to flex their hours up or down in ways that British workers can be unable or unwilling to do. And their orientation to work is often different, focused on maximising earnings and experience rather than achieving a work-life balance. There is also evidence that some migrants work in the social care sector to gain a toe-hold in the UK labour market or as a stepping stone to other jobs. Employers report that migrants sometimes have qualifications and experience in areas allied to care work, including nursing. For example, in research carried out by NIESR and CIPD in 2017 a care home employer said their EU staff include graduates in relevant subjects such as psychology. In comparison, British applicants were reported to be often underqualified educationally for the work and less mature, reflected in poor reliability and work motivation.
It might be argued that more motivated, higher quality workers would be attracted to the sector and also work longer hours if pay were increased, but employers report tight limits in their ability to raise pay. Studies by NIESR and by the LSE find that the introduction of the National Living Wage has failed to improve the sector’s recruitment difficulties and has even reduced the quality of care. If this hasn’t led to a change in the funding model, is it realistic to expect that the end of free movement will?
Immigration isn’t just about numbers
The MAC recommends a scheme for agriculture, but not for social care and the only other routes proposed for low skilled workers are a youth mobility scheme and family members of other visa holders. Neither of these is likely to draw sufficient numbers into care homes: the sector is crying out for motivated individuals with a caring attitude, not 18 year olds on a gap year. The MAC’s reason for making no provision for the sector is that it ‘needs a policy wider than just migration policy to fix its many problems’. And it places the problem at the door of a social care funding model which forces employers to pay at the lowest possible rates in order to make services viable. The MAC expresses concern that
‘Special immigration schemes for social care will struggle to retain enough migrants in the sector if work in it is not made more attractive’.
While this is a fair point, it fails to recognise the role of factors other than pay in the sector’s recruitment difficulties. It also fails to acknowledge the specific contribution that migrants have made to the sector. Rather than substituting for British labour, they have filled skills and labour gaps. They have also benefited colleagues who are less able or willing to be flexible in their hours. And they have brought new experience and perspectives to the teams in which they work, as found by earlier NIESR research. Immigration policy should be informed by these wider benefits, not just whether or not a British person might do the work if wages were higher.
As the MAC report acknowledges, the sector’s short-comings are not due to migration and jobs should be made more attractive regardless. But our ageing population is placing pressure on the care system right now and progress is unlikely to be fast enough. The last thing the system needs is a migration policy that will make its problems worse by not allowing it to recruit the skills and labour it so badly needs.
Heather Rolfe discusses the report’s findings with co-author David Nguyen in a new podcast here.